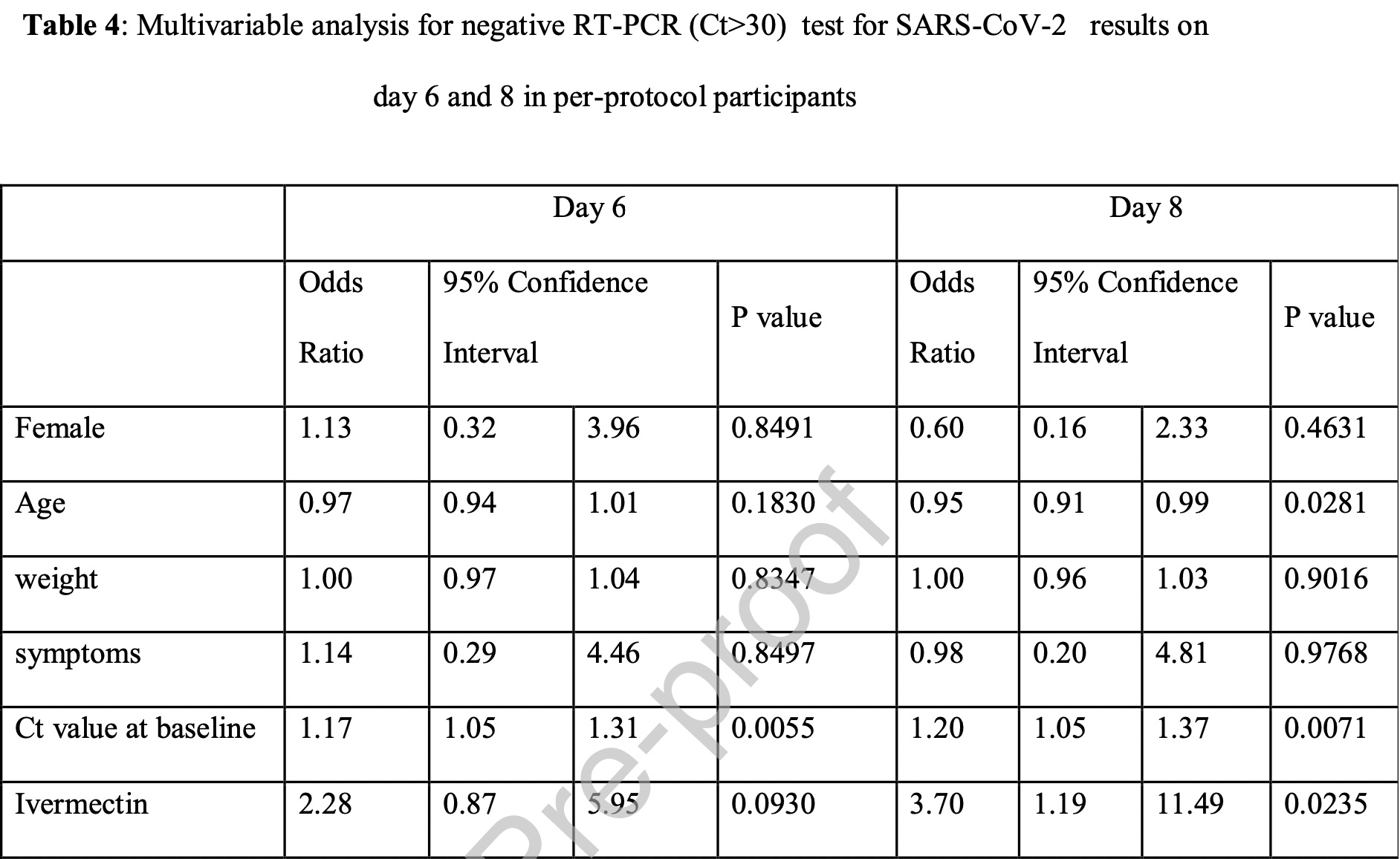
The effect of ivermectin on the viral load and culture viability in early treatment of nonhospitalized patients with mild COVID-19 – a double-blind, randomized placebo-controlled trial
Asaf Biber, Geva Harmelin, Dana Lev, Li Ram, Amit Shaham, Ital Nemet, Limor Kliker, Oran Erster, Michal Mandelboim, Eli Schwartz
International Journal of Infectious Diseases, doi:10.1016/j.ijid.2022.07.003
The effect of ivermectin on the viral load and culture viability in early treatment of non-hospitalized patients with mild COVID-19 -A double-blind, randomized placebo-controlled trial,
☐The authors declare the following financial interests/personal relationships which may be considered as potential competing interests:
References
Basso, Aita, Navaglia, Franchin, Fioretto et al., SARS-CoV-2 RNA identification in nasopharyngeal swabs: issues in pre-analytics, Clin Chem Lab Med,
doi:10.1515/cclm-2020-0749Biancofiore, Mirijello, Puteo, Di Viesti, Labonia et al., Remdesivir significantly reduces SARS-CoV-2 viral load on nasopharyngeal swabs in hospitalized patients with COVID-19: A retrospective case-control study, Journal of Medical Virology,
doi:10.1002/jmv.27598Bray, Rayner, Noël, Jans, Wagstaff, Ivermectin and COVID-19: A report in Antiviral Research, widespread interest, an FDA warning, two letters to the editor and the authors' responses, Antiviral Res,
doi:10.1016/j.antiviral.2020.104805Brown, Chand, Andrews, Auckland, Beshir, Snapshot PCR surveillance for SARS-CoV-2 in hospital staff in England, J Infect,
doi:10.1016/j.jinf.2020.06.069Bryant, Lawrie, Dowswell, Fordham, Mitchell et al., Ivermectin for Prevention and Treatment of COVID-19 Infection: A Systematic Review, Meta-analysis, and Trial Sequential Analysis to Inform Clinical Guidelines, Am J Ther,
doi:10.1097/MJT.0000000000001402Bullard, Dust, Funk, Strong, Alexander et al., Predicting Infectious Severe Acute Respiratory Syndrome Coronavirus 2 From Diagnostic Samples, Clin Infect Dis,
doi:10.1093/cid/ciaa638Carroll, Mcnamara, Comparison and correlation of commercial SARS-CoV-2 real-time-PCR assays, Ireland, Euro Surveillance : Bulletin Europeen Sur Les Maladies Transmissibles = European Communicable Disease Bulletin,
doi:10.2807/1560-7917.ES.2021.26.6.2002079Choudhury, Das, Patra, Bhattacharya, Ghosh et al., Exploring the binding efficacy of ivermectin against the key proteins of SARS-CoV-2 pathogenesis: an in silico approach, Future Virology,
doi:10.2217/fvl-2020-0342Eweas, Alhossary, As, Molecular Docking Reveals Ivermectin and Remdesivir as Potential Repurposed Drugs Against SARS-CoV-2, Frontiers in Microbiology,
doi:10.3389/fmicb.2020.592908Fischer, Eron, Holman, Cohen, Fang et al., A phase 2a clinical trial of molnupiravir in patients with COVID-19 shows accelerated SARS-CoV-2 RNA clearance and elimination of infectious virus, Sci Transl Med,
doi:10.1126/scitranslmed.abl7430Gilad, Oran, Itai, Eli, Evaluation of the relationship between quantitative PCR results and cell culturing of SARS2-CoV with respect to symptoms onset and Viral load -a systematic review, MedRxiv,
doi:10.1101/2021.08.23.21262162Götz, Magar, Dornfeld, Giese, Pohlmann et al., Influenza A viruses escape from MxA restriction at the expense of efficient nuclear vRNP import, Sci Rep,
doi:10.1038/srep23138Hill, Mirchandani, Pilkington, Ivermectin for COVID-19: Addressing Potential Bias and Medical Fraud, Open Forum Infect Dis,
doi:10.1093/ofid/ofab645Lefferts, Blake, Bruden, Hagen, Hodges et al., Nuclear import and export inhibitors alter capsid protein distribution in mammalian cells and reduce Venezuelan Equine Encephalitis Virus replication, MMWR Morb Mortal Wkly Rep,
doi:10.15585/mmwr.mm7108a3Padhy, Mohanty, Das, Meher, Therapeutic potential of ivermectin as add on treatment in COVID 19: A systematic review and meta-analysis, Journal of Pharmacy & Pharmaceutical Sciences : A Publication of the Canadian Society for Pharmaceutical Sciences,
doi:10.18433/jpps31457Poopalasingam, Korenkov, Ashurov, Strobel, Fish et al., Ivermectin: a multifaceted drug of Nobel prize-honoured distinction with indicated efficacy against a new global scourge, COVID-19, New Microbes and New Infections,
doi:10.2139/ssrn.4000128Schwartz, Does Ivermectin have a place in the treatment of mild Covid-19? New Microbes and New Infections
Siedner, Tay, Myf, Fraser, Chan et al., Nuclear localization of dengue virus (DENV) 1-4 non-structural protein 5; protection against all 4 DENV serotypes by the inhibitor Ivermectin, Open Forum Infectious Diseases,
doi:10.1093/ofid/ofab318Wagstaff, Sivakumaran, Heaton, Harrich, Jans, Ivermectin is a specific inhibitor of importin α/β-mediated nuclear import able to inhibit replication of HIV-1 and dengue virus, Biochem J,
doi:10.1042/BJ20120150Wu, Mcgoogan, Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72 314 Cases From the Chinese Center for Disease Control and Prevention, JAMA,
doi:10.1001/jama.2020.2648Wölfel, Corman, Guggemos, Seilmaier, Zange et al., Virological assessment of hospitalized patients with COVID-2019, Nature,
doi:10.1038/s41586-020-2196-xZein, Sulistiyana, Raffaelo, Pranata, Ivermectin and mortality in patients with COVID-19: A systematic review, meta-analysis, and meta-regression of randomized controlled trials, Diabetes Metab Syndr n.d,
doi:10.1016/j.dsx.2021.102186Zhang, Song, Ci, Ju, Li, Ivermectin inhibits LPS-induced production of inflammatory cytokines and improves LPS-induced survival in mice, Inflamm Res,
doi:10.1007/s00011-008-8007-8DOI record:
{
"DOI": "10.1016/j.ijid.2022.07.003",
"ISSN": [
"1201-9712"
],
"URL": "http://dx.doi.org/10.1016/j.ijid.2022.07.003",
"alternative-id": [
"S120197122200399X"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0001-6007-0383",
"affiliation": [],
"authenticated-orcid": false,
"family": "Biber",
"given": "Asaf",
"sequence": "first"
},
{
"affiliation": [],
"family": "Harmelin",
"given": "Geva",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Lev",
"given": "Dana",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ram",
"given": "Li",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-2899-1665",
"affiliation": [],
"authenticated-orcid": false,
"family": "Shaham",
"given": "Amit",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Nemet",
"given": "Ital",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kliker",
"given": "Limor",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-4839-8997",
"affiliation": [],
"authenticated-orcid": false,
"family": "Erster",
"given": "Oran",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mandelboim",
"given": "Michal",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Schwartz",
"given": "Eli",
"sequence": "additional"
}
],
"container-title": "International Journal of Infectious Diseases",
"container-title-short": "International Journal of Infectious Diseases",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2022,
7,
8
]
],
"date-time": "2022-07-08T06:07:31Z",
"timestamp": 1657260451000
},
"deposited": {
"date-parts": [
[
2022,
7,
8
]
],
"date-time": "2022-07-08T06:07:32Z",
"timestamp": 1657260452000
},
"indexed": {
"date-parts": [
[
2022,
7,
8
]
],
"date-time": "2022-07-08T06:43:46Z",
"timestamp": 1657262626366
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2022,
7
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
7,
1
]
],
"date-time": "2022-07-01T00:00:00Z",
"timestamp": 1656633600000
}
},
{
"URL": "http://creativecommons.org/licenses/by-nc-nd/4.0/",
"content-version": "vor",
"delay-in-days": 2,
"start": {
"date-parts": [
[
2022,
7,
3
]
],
"date-time": "2022-07-03T00:00:00Z",
"timestamp": 1656806400000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S120197122200399X?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S120197122200399X?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"prefix": "10.1016",
"published": {
"date-parts": [
[
2022,
7
]
]
},
"published-print": {
"date-parts": [
[
2022,
7
]
]
},
"publisher": "Elsevier BV",
"reference-count": 0,
"references-count": 0,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S120197122200399X"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Infectious Diseases",
"Microbiology (medical)",
"General Medicine"
],
"subtitle": [],
"title": "The effect of ivermectin on the viral load and culture viability in early treatment of non-hospitalized patients with mild COVID-19 – A double-blind, randomized placebo-controlled trial",
"type": "journal-article"
}